
Breaking News
 Economist Issues a Chilling Warning (You Should Prepare)
Economist Issues a Chilling Warning (You Should Prepare)
 The Internet Is Getting Harder to Trust | Josh Smith From #485 | The Way I Heard It
The Internet Is Getting Harder to Trust | Josh Smith From #485 | The Way I Heard It
 DIY LFP Battery Explosion! Is it Possible??
DIY LFP Battery Explosion! Is it Possible??
 House Leadership Delays Vote on Ending the Iran War
House Leadership Delays Vote on Ending the Iran War
Top Tech News
 Cars Are Fast Becoming Dystopian Prison Pods...
Cars Are Fast Becoming Dystopian Prison Pods...
 Our Emergency Water Plan Wasn't Good Enough - So We Built This
Our Emergency Water Plan Wasn't Good Enough - So We Built This
 Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
 Juiced Bikes proves capable electric motorcycles don't have to cost a lot
Juiced Bikes proves capable electric motorcycles don't have to cost a lot
 Headlight projectors turn your car into a drive-in theater
Headlight projectors turn your car into a drive-in theater
 US To Develop Small Modular Nuclear Reactors For Commercial Shipping
US To Develop Small Modular Nuclear Reactors For Commercial Shipping
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
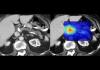 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Can Lowering Inflammation Help Major Depression?

Story at-a-glance
New research data adds to mounting evidence that depression is linked to an inflammatory response
Inflammation influences the quality of sleep, metabolism, stress response and the release of cytokines
Antidepressant medications are associated with significant and dangerous side effects, including violence, aggression and suicide
The senior population is especially vulnerable; the rate of antidepressant drug prescriptions for this group has doubled since 1990, increasing the risk of cognitive decline, dementia, osteoporosis, Type 2 diabetes and heart disease
Effective nonpharmacological options for treatment include exercising, reducing sugar intake, and using light therapy for 30 minutes each day
It is estimated that 7.1% of the adult population in the U.S. experienced at least one major depressive episode in 2017. The highest rates are among those ages 18 to 25 years. Many people believe depression is caused by a chemical imbalance in the brain. This is a theory that has been widely promoted by drug companies and psychiatrists, to the point it is now accepted as fact.
However, this is just a theory and, worse, it's a theory that has been largely discredited. The idea spread quickly after it was proposed in the 1960s when it appeared antidepressant drugs altered brain chemicals. In the 1980s, Prozac (fluoxetine) was released by Eli Lilly and heavily promoted to balance brain chemicals and affect depression.
Prozac had fewer side effects than some of the earlier antidepressants and soon became the poster child for selective serotonin reuptake inhibitor (SSRI) class of antidepressants. However, while heavily prescribed, data repeatedly showed SSRIs worked no better than placebos for those experiencing mild to moderate depression.
Although antidepressants don't effectively treat depression, they do double the risk of harm from suicide and violence in healthy adults and increase aggression in children and adolescents.
Researchers also suggest major depression could be vastly overdiagnosed and overtreated with antidepressants. The majority who are prescribed these drugs end up staying on them long-term, which may compromise their health.
More Studies Link Depression to Inflammation
Researchers have found yet another link between inflammation and depression. In one study1 published in the Journal of Neurology, Neurosurgery & Psychiatry, researchers systematically reviewed the safety and effectiveness of anti-inflammatory agents in people suffering with major depression.
The literature review included results from 30 randomized control trials with a 1,610 participants. In an overall analysis of 26 studies, the researchers found anti-inflammatory agents reduced depressive disorder when compared with placebo. They found no differences in quality of life analysis but did find gastrointestinal event differences between the treatment periods.
A subanalysis of the data demonstrated an adjunctive treatment with antidepressants with nonsteroidal anti-inflammatory drugs, statins, omega-3 FAs and minocycline significantly reduced depressive symptoms.2
Results from another large metanalysis3 carried out by researchers from Aarhus University Hospital in Denmark revealed similar findings, showing anti-inflammatories may be effective in the treatment of depression. One researcher explains the study showed the combination of anti-inflammatory drugs along with antidepressants have beneficial effects.
The results also showed the effect against depression was present when the anti-inflammatory medication was used alone, compared against a placebo. The scientists analyzed 36 international studies of participants who suffered from depression or who had symptoms of depression. One of the researchers, Dr. Ole Köhler-Forsberg, commented on the results of the study:4
"This definitely bolsters our chances of being able to provide personalised treatment for individual patients in the longer term. Of course we always have to weigh the effects against the potential side-effects of the anti-inflammatory drugs.
We still need to clarify which patients will benefit from the medicine and the size of the doses they will require. The findings are interesting, but patients should consult their doctor before initiating additional treatment."
Yet in another recently published study in Molecular Psychiatry5 scientists found patients treated with immunotherapeutics for inflammatory disorders, who also presented with depression or depressive symptoms, experienced symptomatic relief. The team found the reduction in depressive symptoms was not associated with any treatment-related changes in their physical health.



