
Breaking News
 Musk Calls Brain Chips "Jesus-Level" Tech as Neuralink Breakthroughs Advance
Musk Calls Brain Chips "Jesus-Level" Tech as Neuralink Breakthroughs Advance
 Quantum Stocks Erupt As U.S. Gov't Awards $2 Billion, Takes Equity Stakes
Quantum Stocks Erupt As U.S. Gov't Awards $2 Billion, Takes Equity Stakes
 Jobless Claims Refuse To Show Any Signs Of AI Jobpocalypse
Jobless Claims Refuse To Show Any Signs Of AI Jobpocalypse
 Renter Nation Returns? Multi-Family Unit Starts & Permits Soar In April
Renter Nation Returns? Multi-Family Unit Starts & Permits Soar In April
Top Tech News
 Cars Are Fast Becoming Dystopian Prison Pods...
Cars Are Fast Becoming Dystopian Prison Pods...
 Our Emergency Water Plan Wasn't Good Enough - So We Built This
Our Emergency Water Plan Wasn't Good Enough - So We Built This
 Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
 Juiced Bikes proves capable electric motorcycles don't have to cost a lot
Juiced Bikes proves capable electric motorcycles don't have to cost a lot
 Headlight projectors turn your car into a drive-in theater
Headlight projectors turn your car into a drive-in theater
 US To Develop Small Modular Nuclear Reactors For Commercial Shipping
US To Develop Small Modular Nuclear Reactors For Commercial Shipping
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
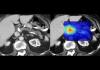 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
U.K. approves CRISPR gene editing to create GMO humans
The gene-editing therapy, which was reportedly designed to treat blood disorders, could appear on the market by as soon as December.
The way CRISPR works is that it functions like a pair of "genetic scissors," chopping up sections of DNA so scientists can edit them by "snipping" specific portions and replacing those portions with new, artificial segments.
According to a 2012 paper that first announced the technology, CRISPR is basically a cheap and easy way to edit genes and create new genetically modified organisms (GMOs) – in this case, out of human beings.
Known as exa-cel therapy, the new CRISPR about to be released, known formally as Casgevy, is the world's first CRISPR therapy for humans to receive approval on the market.
CRISPR's inventers won a Nobel Prize in chemistry in 2020 for the discovery, which in recent years has been used to manipulate plants as a possible solution to "climate change." Only now is CRISPR about to be used on humans, despite the fact that it is highly risky.
Is genetically modifying your body really worth a "cure?"
Casgevy was designed to treat two specific blood conditions: sickle cell disease and beta thalassemia. Also known as sickle cell anemia, the former most commonly occurs in people of African or Caribbean descent and is known to cause debilitating pain.
Beta thalassemia, which can cause mild or severe anemia, is a similar condition that typically requires regular blood transfusions to treat.
Both of these genetic conditions are said to be caused by "errors" in the genes that regulate hemoglobin, a protein that lets red blood cells transport oxygen around the body. Both conditions can also be fatal if left untreated.
Developed by Vertex Pharmaceuticals and CRISPR Therapeutics, the technology was approved after just one study that followed only 29 out of 45 total participants for 16 months. Twenty-eight out of these 29 supposedly had no pain after one year, Nature reported.



