
Breaking News
 White House Correspondents' Dinner Shooter's Link to NASA and Other Curiosities
White House Correspondents' Dinner Shooter's Link to NASA and Other Curiosities
 US Military Ends 72-Year Mandatory Flu Shot Policy
US Military Ends 72-Year Mandatory Flu Shot Policy
 3 Million Ounces of Gold and 28 Million Ounces of Silver Taken Out the Back Door
3 Million Ounces of Gold and 28 Million Ounces of Silver Taken Out the Back Door
Top Tech News
 Researcher wins 1 bitcoin bounty for 'largest quantum attack' on underlying tech
Researcher wins 1 bitcoin bounty for 'largest quantum attack' on underlying tech
 Interceptor-Drone Arms-Race Emerges
Interceptor-Drone Arms-Race Emerges
 A startup called Inversion has introduced Arc, a space-based vehicle...
A startup called Inversion has introduced Arc, a space-based vehicle...
 Mining companies are using cosmic rays to find critical minerals
Mining companies are using cosmic rays to find critical minerals
 They regrew a severed nerve - by shortening a bone.
They regrew a severed nerve - by shortening a bone.
 New Robot Ants Work Like Real Insects To Build And Dismantle On Their Own
New Robot Ants Work Like Real Insects To Build And Dismantle On Their Own
 Russian scientists 'are developing the world's first drug to delay ageing' months after
Russian scientists 'are developing the world's first drug to delay ageing' months after
 Sam Altman's World ID Expands Biometric Identity Checks
Sam Altman's World ID Expands Biometric Identity Checks
 China Tests Directed Energy Beam That Recharges Drones Mid-Flight
China Tests Directed Energy Beam That Recharges Drones Mid-Flight
 Jurassic Park might arrive sooner than expected, just with Dinobots.
Jurassic Park might arrive sooner than expected, just with Dinobots.
No stethoscope for pain: Scientists seek real way to measure
WASHINGTON (AP) — Is the pain stabbing or burning? On a scale from 1 to 10, is it a 6 or an 8?
Over and over, 17-year-old Sarah Taylor struggled to make doctors understand her sometimes debilitating levels of pain, first from joint-damaging childhood arthritis and then from fibromyalgia.
"It's really hard when people can't see how much pain you're in, because they have to take your word on it and sometimes, they don't quite believe you," she said.
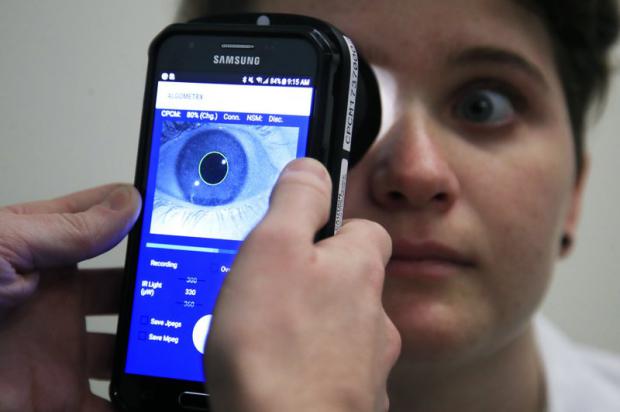
Now scientists are peeking into Sarah's eyes to track how her pupils react when she's hurting and when she's not — part of a quest to develop the first objective way to measure pain.
"If we can't measure pain, we can't fix it," said Dr. Julia Finkel, a pediatric anesthesiologist at Children's National Medical Center in Washington, who invented the experimental eye-tracking device.
At just about every doctor's visit you'll get your temperature, heart rate and blood pressure measured. But there's no stethoscope for pain. Patients must convey how bad it is using that 10-point scale or emoji-style charts that show faces turning from smiles to frowns.
That's problematic for lots of reasons. Doctors and nurses have to guess at babies' pain by their cries and squirms, for example. The aching that one person rates a 7 might be a 4 to someone who's more used to serious pain or genetically more tolerant. Patient-to-patient variability makes it hard to test if potential new painkillers really work.
Nor do self-ratings determine what kind of pain someone has — one reason for trial-and-error treatment. Are opioids necessary? Or is the pain, like Sarah's, better suited to nerve-targeting medicines?
"It's very frustrating to be in pain and you have to wait like six weeks, two months, to see if the drug's working," said Sarah, who uses a combination of medications, acupuncture and lots of exercise to counter her pain.

 Palantir and the New Order
Palantir and the New Order


