
Breaking News
 The Quiet Collapse Under The Market's Surface...It's Getting Louder
The Quiet Collapse Under The Market's Surface...It's Getting Louder
 Buried documents reveal everything...
Buried documents reveal everything...
 Democrats Hopeful Average Texas Voter Wants To Ban Steak And Thinks God Is Gay
Democrats Hopeful Average Texas Voter Wants To Ban Steak And Thinks God Is Gay
 SURVEILLANCE STATE BEING CONSTRUCTED
SURVEILLANCE STATE BEING CONSTRUCTED
Top Tech News
 Cars Are Fast Becoming Dystopian Prison Pods...
Cars Are Fast Becoming Dystopian Prison Pods...
 Our Emergency Water Plan Wasn't Good Enough - So We Built This
Our Emergency Water Plan Wasn't Good Enough - So We Built This
 Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
 Juiced Bikes proves capable electric motorcycles don't have to cost a lot
Juiced Bikes proves capable electric motorcycles don't have to cost a lot
 Headlight projectors turn your car into a drive-in theater
Headlight projectors turn your car into a drive-in theater
 US To Develop Small Modular Nuclear Reactors For Commercial Shipping
US To Develop Small Modular Nuclear Reactors For Commercial Shipping
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
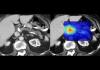 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
The mitochondria are more than just the "powerhouse of the cell" – they initiate immune...
For decades, mitochondria have been relegated to the role of mere "powerhouses of the cell," churning out energy while the immune system's more glamorous players—white blood cells, antibodies, and cytokines—took center stage. But groundbreaking research is shattering this narrow view, revealing mitochondria as master regulators of immunity, orchestrating defenses against bacterial invaders with precision. Far from being passive energy factories, these tiny organelles act as cellular watchtowers, detecting microbial threats and triggering life-saving counterattacks. The implications are staggering: dysfunctional mitochondria may explain why autoimmune patients suffer recurrent infections, and boosting mitochondrial function could revolutionize infection treatment.
Key points:
Mitochondria act as metabolic sensors, detecting bacterial byproducts like lactate to initiate immune responses.
Neutrophils, the body's first responders, rely on mitochondrial signals to deploy sticky DNA traps (NETs) that ensnare and kill bacteria.
Dysfunctional mitochondria in lupus patients impair NET production, leaving them vulnerable to infections despite an overactive immune system.
The discovery opens doors for therapies that enhance mitochondrial sensing to fight infections or suppress harmful immune overreactions.
Nourishing the mitochondria with herbal medicines and phytonutrient-based therapies could empower patients struggling with compromised immune function.
The immune system's hidden command center
Neutrophils, the most abundant white blood cells, are the immune system's rapid-response team, rushing to infection sites to engulf and destroy pathogens. One of their deadliest weapons is the neutrophil extracellular trap (NET)—a spiderweb-like mesh of DNA and toxic proteins that traps bacteria like flies in amber. Until now, scientists believed NETs were triggered primarily by cellular damage. But new research reveals a far more sophisticated system: mitochondria act as metabolic spies, intercepting bacterial distress signals and ordering NET deployment.
The key to this communication? Lactate—a molecule long associated with muscle fatigue but now exposed as a bacterial SOS signal. Many pathogens, including Staphylococcus aureus, excrete lactate as they metabolize nutrients inside immune cells. When mitochondria detect this lactate, they sound the alarm, prompting neutrophils to eject NETs and expel the trapped microbes for other immune cells to finish off. Block this mitochondrial sensing, and bacteria slip through the defenses like thieves in the night.
When mitochondria fail: The autoimmune connection
This discovery sheds light on a cruel paradox: why patients with systemic lupus erythematosus (SLE)—a disease marked by hyperactive immunity—suffer relentless infections. The answer lies in their mitochondria. In lupus patients, these organelles grow deaf to bacterial lactate, failing to trigger NET production. The result? Pathogens replicate unchecked, while the immune system remains stuck in a self-destructive loop, attacking the body instead of invaders.



