
Breaking News
 TICKS! "THE POOR MAN'S NUKE!" - 'They' Figured out how to get to RURAL AMERICA
TICKS! "THE POOR MAN'S NUKE!" - 'They' Figured out how to get to RURAL AMERICA
 15.7% of private credit loans are marked below 80% of principal. More than 10% are below 50%.
15.7% of private credit loans are marked below 80% of principal. More than 10% are below 50%.
 Solid State Batteries are FINALLY Here - I tested EVERYTHING! (PUBLISHER RECOMMENDED)
Solid State Batteries are FINALLY Here - I tested EVERYTHING! (PUBLISHER RECOMMENDED)
Top Tech News
 Cars Are Fast Becoming Dystopian Prison Pods...
Cars Are Fast Becoming Dystopian Prison Pods...
 Our Emergency Water Plan Wasn't Good Enough - So We Built This
Our Emergency Water Plan Wasn't Good Enough - So We Built This
 Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
Sodium Ion Batteries Can Reach 100 Gigawatt Per Hour Per Year Scale in 2027
 Juiced Bikes proves capable electric motorcycles don't have to cost a lot
Juiced Bikes proves capable electric motorcycles don't have to cost a lot
 Headlight projectors turn your car into a drive-in theater
Headlight projectors turn your car into a drive-in theater
 US To Develop Small Modular Nuclear Reactors For Commercial Shipping
US To Develop Small Modular Nuclear Reactors For Commercial Shipping
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
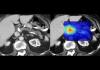 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
A single inflammatory switch may help repair the liver
Signals from the gut make the situation worse by encouraging immune cells to release harmful molecules. Macrophages and monocytes are central players, intensifying injury and shifting the body's defenses toward a more aggressive state. Among them, liver macrophages are essential and are now being explored as therapeutic targets.
Another key factor is Platelet-Activating Factor (PAF), a chemical that drives inflammation, clotting, and changes in blood vessels. In cirrhosis, a serious and ongoing condition, healthy liver tissue is slowly replaced by scar tissue. This replacement causes a loss of structure and function. Liver macrophages create high levels of PAF and its receptor, which raises portal vein pressure and decreases blood pressure in other areas.
Current treatments for liver disease are limited. They mainly tackle complications instead of the root causes of damage. This highlights the need for more research to better understand how the disease works and to create stronger, more effective therapies.
Researchers at Miguel Hernández University in Spain have found a promising way to lessen liver damage and improve blood vessel function in cirrhosis.
"Our main objective was to understand the role of platelet-activating factor (PAF) and its receptor (PAF-R) in liver cirrhosis, a disease characterized by progressive liver damage accompanied by intense chronic inflammation," explained study lead Rubén Francés Guarinos. "The study also evaluated whether blocking this inflammatory pathway could be an effective strategy to improve liver function in cirrhosis."
The researchers looked at both patients with cirrhosis and mice with chemically induced cirrhosis. Some of the mice were given treatments: either a drug that blocks PAF-R receptor, or a DNA methylation inhibitor, for two weeks before surgery (laparotomies).
Researchers then examined liver immune cells to determine how their DNA activity was regulated and measured levels of a key receptor. They also tested liver cells called Kupffer cells by exposing them to PAF and other triggers and measuring the amount of inflammatory molecules they produced. Finally, the team measured markers of liver damage to understand how these treatments and signals affected disease progression.
The study found that in cirrhosis, a change in gene regulation, specifically the removal of chemical marks from the PAF-R gene, causes the gene to become overactive. As a result, liver immune cells produce more PAF-R receptors, which intensifies inflammation and worsens liver damage.
Notably, the researchers showed that blocking PAF with a drug called BN-52021 not only reduced liver injury and improved blood vessel function in cirrhotic mice, but also restored balance in the liver's immune and inflammatory responses.
"Taken together, these findings suggest that drugs capable of blocking PAF action, such as BN-52021, could represent a new therapeutic line for liver cirrhosis," said UMH researcher Enrique Ángel Gomis.

 Tucker Unmasks Hegseth
Tucker Unmasks Hegseth

