
Breaking News
 First hydrogen helicopter just proved it can fly a real mission
First hydrogen helicopter just proved it can fly a real mission
 An Armed Robbery of the World's Energy Supply
An Armed Robbery of the World's Energy Supply
 US Has Lost In Iran. Now Comes The Pain.
US Has Lost In Iran. Now Comes The Pain.
Top Tech News
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
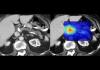 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
A multi-terrain robot from China is going viral, not because of raw speed or power...
 The World's Biggest Fusion Reactor Just Hit A Milestone
The World's Biggest Fusion Reactor Just Hit A Milestone
 Wow. Researchers just built an AI that can control your body...
Wow. Researchers just built an AI that can control your body...
 Google Chrome silently installs a 4 GB AI model on your device without consent
Google Chrome silently installs a 4 GB AI model on your device without consent
 The $5 Battery That Never Dies - Edison Buried This 100 Years Ago
The $5 Battery That Never Dies - Edison Buried This 100 Years Ago
Menopause and gut health: Decoding the relationship between hormones and digestive issues
However, one frequently overlooked aspect of this transitional phase is its profound impact on digestive health. Research indicates that women over 45 are statistically more likely to suffer from more severe gas, bloating, nausea and other gastrointestinal (GI) issues, including weight gain. This phenomenon is particularly concerning as it can significantly impact daily life, beyond the commonly discussed symptoms like irritability and anxiety. Understanding this link between hormonal shifts and digestive distress is increasingly important, especially with a growing population of women entering these life stages.
The hormonal connection: Estrogen decline and gut health
The decline in estrogen levels during menopause plays a pivotal role in the rise of digestive issues. Estrogen, the primary female sex hormone, affects not only reproductive health but also digestive function. As women approach menopause, their ovaries produce less estrogen, leading to systemic changes that can disrupt the delicate balance of the gastrointestinal tract. According to Gretchen Lidicker, M.S., author of "CBD Oil Everyday Secrets" and "Magnesium Everyday Secrets," "these hormonal fluctuations can alter gut bacteria composition and slow down digestion, resulting in symptoms such as bloating and constipation." Research has shown that periods of declining ovarian hormones are associated with an increase in GI symptoms, suggesting that estrogen withdrawal may directly or indirectly contribute to digestive discomfort.
Racial and ethnic disparities in GI symptoms
While menopause affects all women, the experience of GI symptoms is not uniform across different racial and ethnic groups. A study published in Menopause analyzed data from over 1,000 women and found significant differences in the prevalence and severity of GI symptoms based on race and ethnicity. Asian participants reported fewer and less severe GI symptoms, whereas non-Hispanic white women experienced higher total severity scores, especially for nausea, vomiting, diarrhea and loss of appetite. Hispanic women were more likely to report higher severity for constipation, weight gain and bloating. These racial and ethnic disparities highlight the need for personalized approaches to managing GI symptoms during menopause, acknowledging the complex interplay between hormones, genetics and environment.
The role of stress: Amplifying menopausal digestive issues
Stress, a common companion during menopause, further exacerbates digestive issues. As cortisol, often referred to as the "stress hormone," increases during menopause, it can lead to changes in digestive function. Stress triggers the release of adrenaline, which can disrupt the gastrointestinal system, leading to symptoms like bloating, gas and constipation. Many women find that their digestive issues worsen during particularly stressful periods, creating a challenging cycle to break. By addressing stress through relaxation techniques, mindfulness and physical activity, women can help mitigate the exacerbation of GI symptoms during menopause.

 #642: The Tehran Tollbooth
#642: The Tehran Tollbooth
 That is not a real fish. IT'S A ROBOT.
That is not a real fish. IT'S A ROBOT.

